If you’re wondering how much folic acid for pregnancy, the standard recommendation is 400 to 600 micrograms (mcg) per day from supplements, plus food sources. Health experts like the CDC and WHO advise this to support a healthy pregnancy. Always check with your doctor for personalized advice.
Folic acid, a form of vitamin B9, plays a key role in preventing birth defects and supporting your baby’s growth. During pregnancy, your body needs more of it because it helps form the neural tube, which becomes the brain and spine. Without enough, risks like neural tube defects can rise. That’s why starting folic acid early—even before you conceive—is crucial.

In this 2026 guide, we’ll cover everything from dosages by trimester to natural sources and when higher amounts might be needed. We’ll also touch on long-tail topics like how much folic acid during pregnancy first trimester and 400 mcg vs 600 mcg folic acid pregnancy. Remember, while guidelines are based on solid research, your healthcare provider knows your unique needs. Getting the right amount can make a big difference in your pregnancy journey, helping you feel confident and prepared.
How Much Folic Acid Is Recommended During Pregnancy?
The recommended amount of folic acid during pregnancy is generally 400 to 600 mcg per day from a supplement. This comes from trusted sources like the U.S. Preventive Services Task Force and the American College of Obstetricians and Gynecologists. The goal is to reach about 600 mcg of dietary folate equivalents (DFE) total, which accounts for folic acid being more easily absorbed than natural folate from food.
For the standard dosage, most pregnant women should aim for 400 mcg of folic acid in their prenatal vitamin. This is enough for healthy pregnancies without complications. It’s simple and effective, backed by studies showing it reduces birth defect risks.
In the first trimester, the need is especially important. This is when the baby’s neural tube forms, usually in the first 28 days—often before you even know you’re pregnant. So, how much folic acid during pregnancy first trimester? Stick to the 400 to 600 mcg range, but your doctor might suggest starting higher if you’re at risk.
Why Is Folic Acid Important During Pregnancy?
Folic acid is vital during pregnancy because it helps prevent neural tube defects (NTDs). These are serious birth defects affecting the brain and spine, like spina bifida or anencephaly. Scientific studies, including large reviews from the Cochrane Database, show that getting enough folic acid can reduce NTD risks by up to 70%. It works by supporting DNA synthesis and cell division, which are rapid during early fetal development.
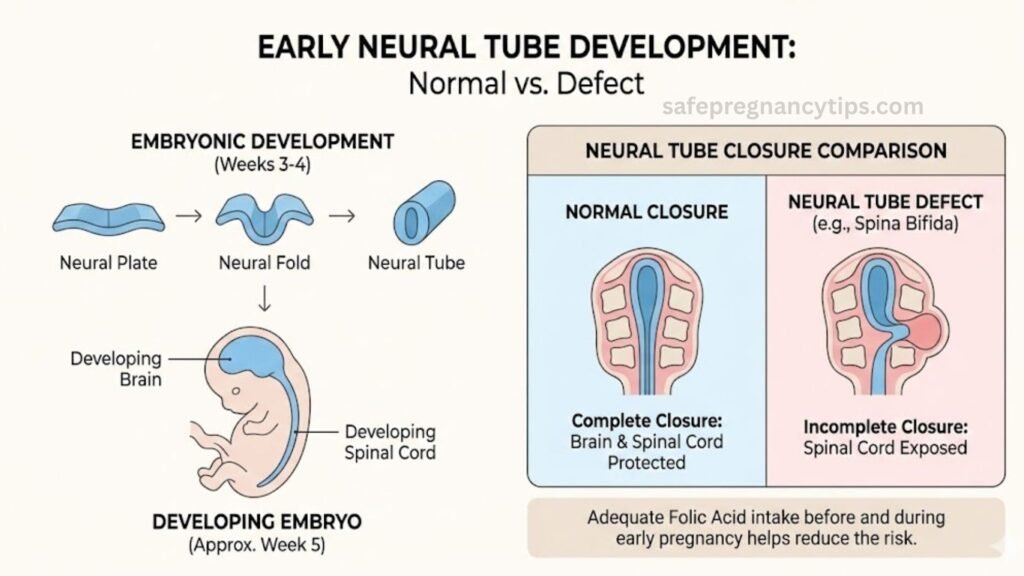
Beyond NTDs, folic acid supports brain and spine development. The neural tube closes early in pregnancy, and adequate levels ensure proper formation. Without it, cells don’t divide correctly, leading to gaps or malformations. This is why timing is key—folic acid needs to be in your system right from the start.
How Much Folic Acid Before Pregnancy?
Starting folic acid before pregnancy is one of the best steps you can take. Experts recommend beginning at least one month before trying to conceive. This builds up levels in your body, ready for when conception happens. Many pregnancies are unplanned, so if you’re of childbearing age, daily folic acid is advised year-round.
The folic acid before pregnancy dosage is typically 400 mcg per day. This matches the general recommendation for women planning to get pregnant. It’s the same as in prenatal vitamins, making it easy to transition once you’re expecting. Studies from the Mayo Clinic show that this pre-conception habit significantly cuts NTD risks.
Folic Acid Dosage by Trimester
Folic acid needs stay fairly steady throughout pregnancy, but let’s break it down by trimester.
In the first trimester, focus on 400 to 600 mcg daily. This is critical for neural tube closure. Comparing 400 mcg vs 600 mcg folic acid pregnancy, both are effective, but 600 mcg covers the RDA for total folate intake. Stick to what your prenatal provides unless advised otherwise.
During the second trimester, maintain the same 400 to 600 mcg. Your baby’s organs are developing, and folic acid supports ongoing cell growth. No big changes here, but keep up with check-ups.
In the third trimester, continue at 400 to 600 mcg. It helps with the baby’s rapid growth and your increased blood needs. Anemia risks can rise now, so folic acid remains important.
What Happens If You Take Too Much Folic Acid?
The safe upper limit for folic acid from supplements is 1,000 mcg per day for adults. This is set by health bodies like the National Institutes of Health to avoid potential issues. Exceeding this regularly isn’t recommended without medical supervision.

Possible side effects from too much include mild digestive upset like nausea, bloating, or gas. In rare cases, it might mask vitamin B12 deficiency symptoms, leading to nerve problems if untreated. But for most people, sticking under 1,000 mcg is safe.
Best Time to Take Folic Acid During Pregnancy
The best time to take folic acid in pregnancy is whenever fits your routine, but consistency matters most. Many prefer morning, as it aligns with breakfast and reduces forgetfulness. Taking it at night is okay too, especially if mornings are rushed. Studies don’t show a big difference in absorption based on time of day.
With food or without? Folic acid absorbs well either way. If it upsets your stomach, pair it with a meal. Avoid taking it with tea or coffee, as they might slightly reduce absorption.
Natural Food Sources of Folic Acid
While supplements are key, natural food sources boost your intake. Spinach is a top choice—one cup cooked provides about 260 mcg of folate. It’s versatile in salads or stir-fries. Lentils offer around 180 mcg per half-cup cooked. They’re protein-packed and great in soups.

Citrus fruits like oranges give 50 mcg per fruit. They’re refreshing and vitamin C-rich. Fortified cereals can have 100-400 mcg per serving. Check labels for added folic acid. Other sources include broccoli, avocados, and eggs. Aim for a varied diet to complement your supplement.
Do All Pregnant Women Need the Same Dose?
No, not all pregnant women need the same folic acid dose—it varies by health factors. For diabetes, higher doses like 4-5 mg might be recommended, as it increases NTD risks. Obesity can affect absorption, so doctors may suggest more than 400 mcg.
If you’ve had a previous miscarriage or NTD-affected pregnancy, 4,000 mcg is often prescribed starting pre-conception.
FAQ
Is 5mg folic acid too much during pregnancy?
For most women, yes—5 mg (5,000 mcg) is much higher than the standard 400-600 mcg and could exceed safe limits without need. However, if you have high-risk factors like a history of neural tube defects or certain medical conditions, your doctor might prescribe 5 mg. Always follow professional advice to avoid side effects.
Can I take 800 mcg daily?
Yes, 800 mcg falls within the recommended range of 400-800 mcg for pregnancy planning or during pregnancy. It’s safe for most and provides a buffer for absorption. Check with your doctor if you have concerns.
How long should I take folic acid?
Start at least one month before conception, continue through the first trimester at minimum, and ideally the whole pregnancy. If breastfeeding, keep going for several months postpartum to support your health and baby’s needs
What if I miss one dose?
Don’t worry—missed doses happen. Take it as soon as you remember, unless it’s almost time for the next. Skip doubling up to avoid excess. Consistency over time is what counts most.
Conclusion:-
In summary, understanding how much folic acid for pregnancy is key to a healthy start. The standard 400-600 mcg daily supports vital development and reduces risks. Incorporate natural sources, time your intake wisely, and adjust for personal factors like high-risk conditions.
Remember topics like folic acid before pregnancy dosage and best time to take folic acid in pregnancy for better planning. With guidelines from 2026, you’re equipped to make informed choices. Prioritize your prenatal visits for tailored guidance. Taking these steps empowers you for a smoother pregnancy journey.
READ MORE:-
Normal vs Abnormal Discharge During Pregnancy Symptoms, Colors & When to See a Doctor
Pregnancy Tips for Normal Delivery: Diet, Exercise, and Best Practices
How to Take Care of Pregnancy in the First 3 Months: A Simple First Trimester Guide










